Sorry, nothing in cart.
Trigeminal Neuralgia Causes, Symptoms and Treatment
- By admin
- |
- General Blog
- |
What is Trigeminal Neuralgia?
Tic douloureux is known as trigeminal neuralgia (TN). It is a chronic pain condition that causes sudden, acute facial pain. It affects the trigeminal nerve, also known as the fifth cranial nerve, which supplies sensation and nerve connection to numerous areas of the head and face.
Causes of Trigeminal Neuralgia:
TN is a form of neuropathic pain that is typically caused by nerve damage or lesion.
- Sudden, severe pain, generally on one side of the face
- Pain attacks that can last anywhere from a few seconds to two minutes
- Numbness or tingling feelings
- searing, throbbing, or painful sensations
- Pain attacks that occur on a regular basis for days to weeks or longer, often many times per day
Nerve Trigeminal Signs and Symptoms:
The trigeminal nerves are cranial nerves that link your brain and brain stem to several areas in your brain, head, trunk, and neck. Each of your body’s and brain’s 12 nerves divides to serve two sides. Each nerve also has three branches that transmit feeling to the top, middle, and bottom of your face.
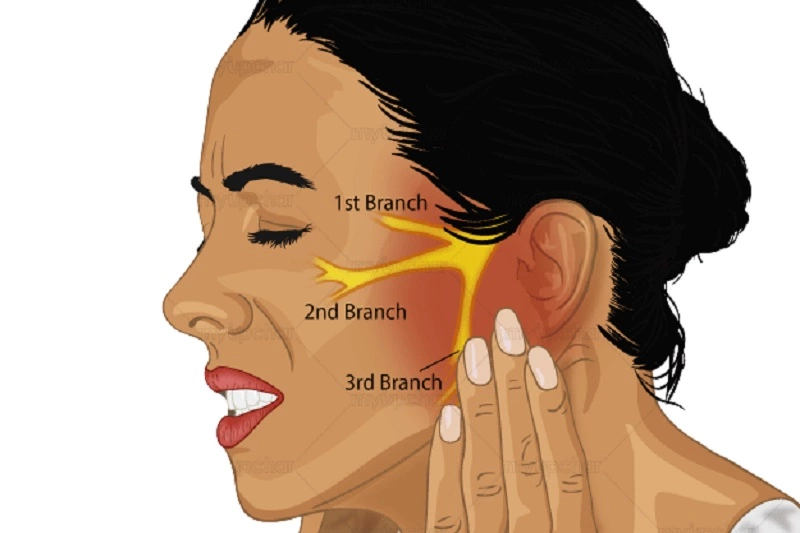
- The ophthalmic, or top, branch of the nerve provides feeling to the majority of your scalp, forehead, and front of your head.
- The maxillary, or middle, branch is responsible for the stimulation of your cheekbones, upper jaw, upper lip, teeth and gums, and the sides of your nose.
- The nerves in your lower jaw, teeth and gums, and lower lip are supplied by the mandibular, or lower, branch.
The condition may damage more than one nerve branch. In rare situations, both sides of your face may be affected at separate periods, or even, less frequently, both sides of your face at the same time (bilateral TN).
There are two main types of Trigeminal neuralgia (TN):
Trigeminal neuralgia Type 1:
This is the “classic” or “typical” form of the health problem. It causes severe, intermittent, sudden burning or shock-like pain in the face. Each episode might run anywhere from a few seconds to two minutes. These bouts can happen fairly close together and can last up to two hours.
Vibration or touch with the cheek (like when shaving, washing your face, or applying makeup), brushing teeth, eating, drinking, talking, or being exposed to wind can all cause strong pain flashes. The pain may be limited to one part of your face or it may spread. Pain attacks are uncommon during sleeping. Because of the severity of the pain, some persons might skip regular activities or social connections in order to avoid a coming attack.
Trigeminal neuralgia Type 2:
This is an “atypical” kind of disease with persistent aching, burning, and stabbing pain. This type of pain is usually less intense than Type 1.
You can have both types of trigeminal neuralgia, sometimes at the same time. The degree of agony can be both mentally and physically debilitating. TN attacks often halt for a short amount of time before returning. In certain situations, the condition is growing, which means that the attacks get worse with time, with fewer and shorter pain-free intervals between them.
The pain-free intervals slowly reduce in progressive TN, and pain medicine becomes less effective.
Who is more likely to get Trigeminal neuralgia (TN)?
TN is most common in those over the age of 50, but it can develop at any age, including infancy. Women are more likely than men to suffer from the disease.
Other conditions that might produce TN include:
As it exits the brain stem, a blood vessel pressures on the trigeminal nerve. The protective layer around the nerve (the myelin sheath) gets worn away or damaged as a result of this compression.
Multiple sclerosis is a disease that causes the myelin sheath of the trigeminal nerve to become thinner.
- Nerve compression is caused by a tumor.
- An arteriovenous malformation is a tangle of arteries and veins.
- Trigeminal nerve injury (perhaps caused by sinus surgery, mouth surgery, stroke, or face trauma)
- Trigeminal neuralgia is diagnosed and treated in the same way.
Trigeminal neuralgia (TN) Diagnosis:
The diagnosis of TN is based mostly on your medical history and symptoms, as well as the findings of physical and neurological testing.
Before TN is diagnosed, additional conditions that cause facial pain should be checked out.
Other conditions that induce face pain include:
- Post-herpetic neuralgia (nerve pain caused by a shingles epidemic)
- Headaches in clusters
- TMJ is a disease that causes discomfort and dysfunction in the jaw joint and the muscles that govern jaw movement.
A magnetic resonance imaging (MRI) brain scan may be ordered to rule out a tumor or multiple sclerosis as the source of your suffering. A blood artery pressing the nerve may or may not be visible on this imaging. Special MRI imaging approaches can detect the existence and level of nerve compression by a blood vessel.
If doctors suspect you have TN1, they may recommend that you take a brief course of antiseizure medication. If the drug helps, it contributes to a TN1 diagnosis.
TN2 diagnosis is more complex and difficult, but doctors may recommend that you try mild dosages of a tricyclic antidepressant drug (such as amitriptyline and nortriptyline) to see if it helps. If this is the case, the positive response to treatment supports a TN2 diagnosis.
Trigeminal Neuralgia (TN) Treatment
People suffering from Trigeminal Neuralgia (TN) require efficient medicinal or surgical pain relief. Medicines, surgery, and complementary therapies are among the treatment options.
Medications
Following numerous medications that can be used to treat trigeminal neuralgia (TN):
Anticonvulsant drugs: (Pregabalin | Gabapentin)
1. Pregabalin 100mg ER
2. Gabapentin 100mg
Anticonvulsants are medications that inhibit nerve activity. They are usually effective in treating trigeminal neuralgia type 1 (TN1) but are frequently effective in treating trigeminal neuralgia Type 2 (TN2). Gabapentin, pregabalin, carbamazepine, oxcarbazepine, topiramate, clonazepam, phenytoin, lamotrigine, and valproic acid are examples of these medications.
Antidepressants:
Pain can be treated with antidepressants such as
1. Duloxetine
2. Escitalopram
3. Sertraline
Opioids: (Tapentadol)
1. Tapfree ER 100mg Tapentadol Tablet
2. Tapal ER 100 mg
Tapentadol (Tapentadol extended-release) Opioid class medicine that is usually effective for treating the sharp, constant pain caused by Trigeminal neuralgia type 1 (TN1). Tapentadol extended-release (Opioid Painkiller) can also aid some people with Trigeminal neuralgia type 2 (TN2).
Surgery
If medicine does not help your pain or causes unbearable side effects such as cognitive difficulties, memory loss, excessive fatigue, bone marrow suppression, or allergy, your doctor may consider surgery. People frequently seek surgical treatment for TN since it is a progressive illness that grows resistant to medicines over time.
What are the most recent improvements in trigeminal neuralgia?
The National Institute of Neurological Disorders and Stroke (NINDS), a component of the National Institutes of Health, funds a wide range of TN research. This research are looking into the factors that cause chronic pain and TN, as well as new diagnostic methods and treatments. Other study focuses on TN through studies related to pain research. The National Institute of Dental and Craniofacial Research also contributes to TN research.
Women are more likely than males to experience pain from TN and other chronic pain syndromes, although the reasons for this are unknown. Researchers are investigating how estrogen hormones may influence nerve pain activities, especially TN pain. Understanding estrogen activity on pain nerves may help explain why women are more prone to pain. This research could also lead to the development of drugs that reduce estrogen activity on nerves that carry pain signals to the brain and spinal cord.
FAQS:
What is the main cause of trigeminal neuralgia?
Pressure on the trigeminal nerve around where it enters the brain stem causes classic trigeminal neuralgia. The brain stem is the base of the brain that connects to the spinal cord. The pressure is usually caused by an artery or vein squashing (compressing) the trigeminal nerve.
What is the primary sign of trigeminal neuralgia?
Trigeminal neuralgia is characterized by sudden occurrences of intense, sharp, shooting facial pain that range from a few seconds to around 2 minutes. The sensation is frequently characterized as intense, similar to an electric shock. The attacks can be so terrible that you are unable to accomplish anything throughout them.
What are the most common treatments for trigeminal neuralgia?
Your doctor will usually prescribe Tapendatol Extended-Release Opioid drugs to reduce or block the pain signals transmitted to your brain in order to treat trigeminal neuralgia. , which has been shown to be beneficial in treating the condition.
How does trigeminal neuralgia feel?
Trigeminal neuralgia is characterized by abrupt, intense face discomfort. It is frequently described as a sudden shooting pain or an electric shock in the jaw, teeth, or gums. It frequently comes in quick, unpredictable bursts that last anywhere from a few seconds to around 2 minutes. The attacks come to an abrupt halt.
Is trigeminal neuralgia ever gone?
The quick answer is that it is unlikely. Trigeminal neuralgia may worsen rather than improve with time. This indicates that you may begin with a milder condition, but it might progress and the pain may worsen over time.
Is it possible for stress to cause trigeminal neuralgia?
While stress does not cause trigeminal neuralgia, it might worsen the problem. There isn’t much known about how or why, but one theory is the link between stress and pain. Chronic pain has been linked to stress-induced pain sensitivity, according to research.
How do you get rid of trigeminal neuralgia pain quickly?
Many people find that applying heat to the affected area relieves their trigeminal neuralgia discomfort. This can be managed locally by using a hot water bottle or other hot compress on the painful area. To accomplish this, microwave a beanbag or dry washcloth. You might also take a hot shower or bath.
 English
English
 French
French  German
German



Leave a Reply